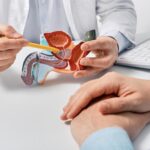
Can You Have Sex With Phimosis?

Allo Health is dedicated to personalized well-being, offering support and trusted information tailored to individual health goals. The platform emphasizes human-generated content, led by a distinguished medical team of experts, including physicians and sexual health specialists. Their commitment to credibility involves rigorous fact-checking, authoritative research, and continuous updates to ensure accurate, up-to-date information. Allo Health's unique approach goes beyond conventional platforms, providing expert-led insights and a continuous commitment to excellence, with user feedback playing a crucial role in shaping the platform's authoritative voice.

Dr Sandip completed his training in Psychiatry and sexual medicine in the UK. A post-graduate in Psychiatry from KMC Manipal, he worked in the UK for over 8 years following a one-year research post at NIMHANS, Bangalore. With an interest in the fields of sexual health and functioning, he has authored articles in books and peer-reviewed journals. A recipient of the student of the year award by BSART in 2010, he is currently a consultant psychiatrist and sexual and relationship therapist with a belief in a holistic and psychotherapeutic approach to treating psychological distress.
Why This Was Upated?
Our experts continually monitor the health and wellness space, and we update our articles when new information became available.
Updated on 14 June, 2024
- Article was updated as part of our commitment to diversity, equity, and inclusion.
"The following blog article provides general information and insights on various topics. However, it is important to note that the information presented is not intended as professional advice in any specific field or area. The content of this blog is for general educational and informational purposes only.
Book consultation
The content should not be interpreted as endorsement, recommendation, or guarantee of any product, service, or information mentioned. Readers are solely responsible for the decisions and actions they take based on the information provided in this blog. It is essential to exercise individual judgment, critical thinking, and personal responsibility when applying or implementing any information or suggestions discussed in the blog."
Sex is an important aspect of human life, and men with phimosis need to know that it is absolutely possible for them to enjoy it just like anyone else. Sex with Phimosis can be difficult, but with the right preparation and information, intimate moments can be enjoyable and fulfilling.
Understanding Phimosis: Causes, Symptoms, and Treatment Options
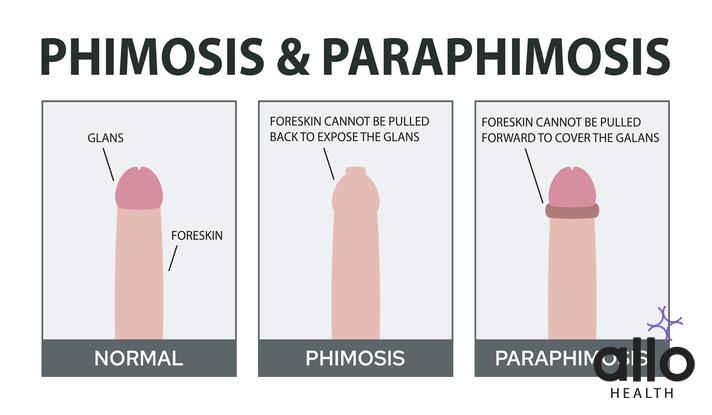
Phimosis is a condition characterized by the inability to retract the foreskin over the glans (head) of the penis. It can occur in males of all ages and is more common in infants and young children. In some cases, it may resolve naturally as a child grows older, but for others, treatment may be necessary. Let’s explore the causes, symptoms, and treatment options for phimosis in detail:
Types Of Phimosis
- Physiological Phimosis: This is the natural condition in infants and young boys where the foreskin cannot be fully retracted. It typically resolves on its own as the child grows older and does not usually cause any concerns.
- Pathological Phimosis: This refers to the condition where the foreskin cannot be retracted due to some underlying medical or anatomical concern. Pathological phimosis can be further categorized into:
- Phimosis with Balanitis: In this case, the foreskin is too tight and cannot be retracted, leading to inflammation of the glans (head) of the penis, known as balanitis. This condition may cause discomfort and pain during sexual activity.
- Scarring Phimosis: This occurs when the foreskin becomes scarred and loses its elasticity, making it difficult to retract. Scarring can result from various factors such as repeated infections, trauma, or inflammatory skin conditions. It may interfere with sexual intercourse and can be accompanied by pain.
- Phimosis due to Preputial Stenosis: Preputial stenosis refers to a narrowing or constriction of the opening of the foreskin. It can make retraction difficult or impossible. Sexual activity may be challenging or uncomfortable in such cases.
Causes of Phimosis
- Congenital Phimosis: Some boys are born with a tight foreskin that does not retract easily. This is often due to adhesions between the foreskin and the glans, which gradually loosen over time.
- Scarring: Injuries, infections, or inflammation of the foreskin or the glans can lead to scarring, causing the foreskin to become tight and difficult to retract.
- Balanitis: This refers to inflammation of the glans and foreskin, often caused by poor hygiene, infections, or certain skin conditions. Chronic balanitis can lead to scarring and phimosis.
- Medical Conditions: Certain medical conditions, such as lichen sclerosus, a chronic skin disorder, can cause the foreskin to become tight and lead to phimosis.
Symptoms of Phimosis
- Difficulty retracting the foreskin over the glans.
- Pain or discomfort during urination.
- Pain or discomfort during sexual activity.
- Redness, swelling, or inflammation of the foreskin or glans.
- Inability to clean the area beneath the foreskin properly, leading to a buildup of smegma (a whitish substance) and increased risk of infections.
Treatment Options for Phimosis
- Observation: In infants and young children, mild cases of phimosis may resolve naturally as they grow older. Regular observation and gentle retraction, if possible, are recommended.
- Topical Steroid Creams: Steroid creams, such as hydrocortisone, can be prescribed to help loosen the foreskin. The cream is applied to the tight area, and gradual improvement is expected over a few weeks.
- Stretching Exercises: Manual stretching of the foreskin can help to gradually widen the opening. This technique is often recommended along with the use of steroid creams.
- Surgical Intervention: In cases where conservative methods fail or if phimosis causes significant discomfort or recurrent infections, surgery may be considered. Two common surgical procedures for phimosis include:
- Circumcision: This involves the surgical removal of the foreskin. It is a permanent solution and is typically performed under local or general anesthesia.
- Preputioplasty: This procedure involves making a small incision in the tight area of the foreskin to widen the opening. It is a less invasive alternative to circumcision and is often preferred in cases where preservation of the foreskin is desired.
The treatment approach for phimosis depends on the severity of the condition, the age of the individual, and the presence of any underlying medical conditions. It is always recommended to consult with a healthcare professional, such as a urologist or pediatrician, who can provide a proper diagnosis and guide you through the most suitable treatment options.
How Phimosis Can Affect Sexual Functioning
Phimosis, which is the inability to retract the foreskin over the glans of the penis, can have an impact on sexual functioning in various ways. Here’s a detailed look at how phimosis can affect sexual function:
- Pain or Discomfort: Phimosis can cause pain or discomfort during sexual activity, particularly during penetration or when the foreskin is forcibly retracted. This can lead to a decrease in sexual pleasure and may even result in avoidance of sexual encounters altogether.
- Difficulty with Penetration: In severe cases of phimosis, where the foreskin is extremely tight and cannot be retracted at all, penetration may be difficult or impossible. This can interfere with sexual intercourse and may cause frustration or anxiety for both partners.
- Increased Risk of Infections: Phimosis can increase the risk of developing infections in the genital area. The inability to clean under the foreskin properly can lead to a buildup of smegma, which is a substance consisting of dead skin cells and other bodily fluids. This can create an environment conducive to bacterial or fungal growth, resulting in infections such as balanitis. Infections can cause discomfort, pain, and may require medical intervention, which can impact sexual functioning.
- Psychological Impact: Phimosis can have psychological effects on individuals. It may lead to feelings of embarrassment, self-consciousness, or low self-esteem, especially if the condition interferes with sexual experiences or relationships. These psychological factors can further contribute to sexual difficulties, including decreased libido, performance anxiety, or difficulties in maintaining intimacy.
- Interference with Ejaculation: In some cases, severe phimosis can interfere with ejaculation. The tightness of the foreskin may restrict the movement of the glans during orgasm, potentially leading to pain or discomfort during ejaculation. This can affect sexual satisfaction and overall sexual functioning.
Not all individuals with phimosis will experience significant sexual difficulties. The impact of phimosis on sexual functioning can vary depending on the severity of the condition, individual differences, and personal preferences. Treatment options for phimosis, such as topical creams, stretching exercises, or surgical interventions, can help alleviate the symptoms and improve sexual function in many cases.
The Psychological Impact of Phimosis on Men and Their Partners
Phimosis, the condition characterized by the inability to retract the foreskin over the glans of the penis, can have psychological impacts not only on men but also on their partners. Here’s a detailed look at the psychological impact of phimosis:
Men’s Psychological Impact
- Embarrassment and Self-consciousness: Men with phimosis may feel embarrassed or self-conscious about their condition, especially in intimate situations. They may worry about how their partner will perceive or react to it, which can lead to a negative body image and reduced self-esteem.
- Performance Anxiety: Phimosis can create performance anxiety related to sexual encounters. The fear of pain or discomfort during sexual activity may result in reduced sexual confidence and an increased focus on potential concerns rather than on pleasure and intimacy.
- Reduced Sexual Satisfaction: Phimosis can diminish sexual satisfaction due to pain, discomfort, or the inability to fully engage in sexual activities. This may lead to frustration, dissatisfaction, and a negative impact on overall sexual well-being.
- Relationship Strain: If phimosis affects sexual functioning or causes distress, it can put strain on intimate relationships. Communication difficulties, feelings of inadequacy, and decreased sexual activity can create tension and emotional distance between partners.
Partners’ Psychological Impact
- Concern and Worry: Partners of men with phimosis may experience concern and worry about their partner’s condition. They may worry about the potential pain or discomfort their partner may experience during sexual activity, leading to a diminished desire for sexual intimacy.
- Feelings of Rejection: Partners may mistakenly perceive the inability to fully retract the foreskin as a lack of interest or attraction towards them. This can result in feelings of rejection or inadequacy, affecting their self-esteem and overall relationship satisfaction.
- Communication Challenges: Discussing phimosis and its impact on sexual functioning can be challenging for both partners. Misunderstandings, discomfort, and difficulties in finding a suitable solution may arise, leading to a breakdown in communication and potential relationship conflicts.
It is encouraged for both the affected individual and their partner to have open and empathetic communication about phimosis. Seeking professional help, such as consulting a healthcare provider or a couples’ therapist, can provide a supportive environment to address concerns, explore treatment options, and enhance understanding between partners.
Treating phimosis through appropriate medical interventions, such as topical creams, stretching exercises, or surgical procedures, can alleviate physical symptoms and potentially reduce the associated psychological impact. Additionally, education about the condition and reassurance from healthcare professionals can help individuals and their partners develop a better understanding of phimosis and its management.
Remember, every individual’s experience with phimosis and its psychological impact can vary. Seeking professional guidance is crucial in addressing specific concerns and developing strategies to promote psychological well-being for both the affected individual and their partner.
Preparing for Sex with Phimosis: Tips for Men and Their Partners
Preparing for sexual activity when dealing with phimosis, the condition where the foreskin is tight and cannot be easily retracted, may require some additional considerations and preparations. Here are some tips for men with phimosis and their partners to help make the experience more comfortable and enjoyable:
- Communication: Open and honest communication is key. Both partners should discuss their expectations, concerns, and any potential challenges related to phimosis. This will help create a supportive and understanding environment.
- Gentle Exploration: Before engaging in sexual activity, men with phimosis can gently explore and become familiar with their own bodies. This can involve gradually retracting the foreskin as much as possible without causing discomfort or pain. Understanding the level of retraction and what feels comfortable can help guide sexual activities.
- Lubrication: The use of a water-based lubricant can significantly reduce friction and discomfort during sexual activity. Apply a generous amount of lubricant to the glans and inner foreskin to facilitate smooth movement.
- Foreplay: Engaging in extended periods of foreplay can help relax both partners and increase natural lubrication. It can also assist in gradually stretching the foreskin, making it more pliable and easier to retract.
- Positioning: Experimenting with different sexual positions can help find ones that minimize discomfort and provide the most pleasure. Positions that allow more control over the depth and pace of penetration may be preferred.
- Patience and Gradual Progression: It’s important to take things slowly and listen to the body’s response. If discomfort or pain arises, it’s advisable to pause, adjust, or switch to alternative activities. Gradually increase the level of retraction over time, as the foreskin becomes more flexible and accommodating.
- Relaxation Techniques: Both partners can benefit from practicing relaxation techniques, such as deep breathing, to reduce anxiety and tension. A relaxed state can enhance sexual pleasure and reduce any potential discomfort associated with phimosis.
- Focus on Pleasure and Intimacy: While dealing with the challenges of phimosis, it’s crucial to prioritize pleasure and emotional connection. Expanding the definition of sexual intimacy beyond penetration can help foster a satisfying and fulfilling sexual experience.
- Seeking Professional Help: If phimosis significantly impacts sexual functioning or causes distress, it’s important to seek guidance from a healthcare professional. They can provide appropriate treatment options, address concerns, and offer support tailored to the individual’s needs.
Foreplay Techniques to Make Sex More Comfortable for Men with Phimosis
Engaging in foreplay can be particularly beneficial for men with phimosis, as it helps in relaxation, arousal, and preparing the body for sexual activity. Here are some foreplay techniques that can make sex more comfortable for men with phimosis:
- Communication: Talk openly with your partner about your preferences, boundaries, and any concerns related to phimosis. This will create a supportive and understanding atmosphere and help guide the foreplay activities.
- Sensual Massage: Begin by giving or receiving a sensual massage. This can be a full-body massage or focus on specific erogenous zones, such as the back, neck, thighs, and buttocks. It allows both partners to relax, release tension, and build intimacy.
- Oral Stimulation: Encourage your partner to engage in oral sex, focusing on other erogenous areas besides the glans. This can include gentle licking, kissing, and sucking on the shaft, scrotum, and perineum. It allows for pleasure and arousal without the need for retracting the foreskin.
- Manual Stimulation: Manual stimulation of the penis can provide pleasure and be more comfortable for men with phimosis. Experiment with different techniques, such as using a lubricated hand or incorporating various grips, strokes, and pressures that feel pleasurable and within your comfort zone.
- Focus on Non-Penetrative Activities: Foreplay doesn’t have to be solely focused on penetration. Explore other non-penetrative activities that provide pleasure and intimacy, such as kissing, cuddling, caressing, or engaging in mutual masturbation. This allows both partners to enjoy sexual pleasure without the need for retraction.
- Incorporate Sex Toys: Introducing sex toys into foreplay can enhance pleasure and provide different sensations. Explore options such as vibrators, prostate massagers, or textured sleeves that can be used on the penis to add variety and excitement.
- Use Lubrication: Apply a water-based lubricant to the penis and surrounding areas during foreplay. This reduces friction, enhances comfort, and makes manual or oral stimulation more pleasurable. Experiment with different types of lubricants to find the one that works best for you.
- Experiment with Different Sensations: Try incorporating different sensations during foreplay, such as using ice cubes, feather ticklers, or soft fabrics to explore the erogenous zones. This can enhance arousal and pleasure without the need for retracting the foreskin.
- Take Breaks: If at any point during foreplay you experience discomfort or pain, communicate with your partner and take breaks as needed. Pause, adjust the activity, or switch to a different form of stimulation that is more comfortable.
Remember, every individual’s preferences and comfort levels may vary. It’s essential to communicate openly with your partner, listen to your body, and explore what feels pleasurable and comfortable for you. Taking the time for foreplay and focusing on mutual pleasure and intimacy can contribute to a satisfying and enjoyable sexual experience, even with phimosis.
Best Positions for Sex With Phimosis
When engaging in sexual activity with phimosis, choosing positions that minimize discomfort and allow for better control over the movement of the foreskin can be beneficial. Here are some positions that may be more comfortable for individuals with phimosis:
- Missionary Position: The missionary position can be a good option for men with phimosis. In this position, the man lies on top of the partner while facing each other. This allows for easier control over the depth and pace of penetration, minimizing discomfort.
- Spooning Position: The spooning position involves both partners lying on their sides, with the man positioned behind the partner. This position allows for more shallow penetration and reduces the risk of the foreskin being pulled back too forcefully.
- Woman on Top: In this position, the woman straddles the man and takes control of the rhythm and depth of penetration. This allows the man to be more passive and reduces the chances of the foreskin being retracted too far.
- Side-by-Side Position: The side-by-side position is similar to spooning but with both partners facing the same direction. This position offers more comfort and control, allowing for gradual and gentle penetration without putting excessive strain on the foreskin.
- Modified Doggy Style: In the doggy style position, the man penetrates the partner from behind. However, to accommodate phimosis, the man can adjust the angle and depth of penetration to ensure comfort and avoid pulling the foreskin too far back.
- Oral or Manual Stimulation: Engaging in oral or manual stimulation without penetration can be an alternative option. This allows for pleasure and intimacy without the need for retraction of the foreskin.
Coping with Pain During Sex With Phimosis
Experiencing pain during sex due to phimosis can be distressing and may affect sexual satisfaction and overall well-being. Here are some strategies to cope with pain during sex with phimosis:
- Open Communication: Communicate openly and honestly with your partner about the pain you’re experiencing. Share your concerns, fears, and boundaries. A supportive and understanding partner can help create a safe space and work together towards finding solutions.
- Foreplay and Relaxation: Engage in extended periods of foreplay to increase arousal and natural lubrication. This can help relax the muscles and reduce pain during penetration. Explore sensual massages, kissing, oral stimulation, or other activities that promote relaxation and arousal.
- Lubrication: Use a water-based lubricant to reduce friction and discomfort during sex. Apply a generous amount to the penis and surrounding areas to ensure smooth movement. Experiment with different lubricant brands and types to find the one that works best for you.
- Gradual Penetration: Take it slow and gradually increase the depth of penetration. Focus on finding a pace and depth that feel comfortable for you. If you experience pain, pause and communicate with your partner. Adjust the angle or depth of penetration to reduce discomfort.
- Alternative Forms of Stimulation: If penetration continues to be painful, explore other forms of sexual stimulation that don’t require retraction of the foreskin. Oral sex, manual stimulation, or focusing on other erogenous zones can provide pleasure and maintain intimacy.
- Pain Management Techniques: Practice pain management techniques such as deep breathing, relaxation exercises, or mindfulness. These techniques can help distract from pain and promote a more relaxed state during sexual activity.
- Topical Anesthetics: In consultation with a healthcare professional, consider using topical anesthetics to temporarily numb the sensitive areas and reduce pain during sex. However, it’s essential to use these products as directed and consult with a healthcare professional for proper guidance.
- Seek Professional Help: If the pain persists or causes significant distress, it’s advisable to consult with a healthcare professional, such as a urologist or sexual health specialist. They can assess the underlying causes, provide appropriate treatment options, and address any specific concerns you may have.
When to See a Doctor for Phimosis
It is advisable to consult a healthcare professional, such as a urologist, for an evaluation and guidance if you or your child are experiencing phimosis. Here are some situations when it is recommended to see a doctor for phimosis:
- Difficulty Urinating: If phimosis is causing difficulty in urination, such as a weak urine stream, pain, or discomfort during urination, it is important to seek medical attention. This could indicate a more severe case of phimosis or other underlying concerns.
- Pain or Inflammation: If you or your child experience persistent pain, redness, swelling, or inflammation in the foreskin or glans, it is recommended to consult a doctor. These symptoms may indicate an infection or another medical condition that requires treatment.
- Recurrent Infections: If phimosis is associated with recurrent infections, such as balanitis (inflammation of the glans and foreskin), it is important to seek medical evaluation. Recurrent infections can be a sign of an underlying concern that needs to be addressed.
- Difficulty with Hygiene: If you or your child are unable to clean under the foreskin properly due to the tightness, leading to a buildup of smegma or recurrent infections, it is advisable to see a doctor. Proper hygiene is essential for genital health, and a healthcare professional can provide guidance on cleaning techniques.
- Pain or Discomfort during Sexual Activity: If phimosis is causing pain or discomfort during sexual activity and impacting sexual satisfaction, it is recommended to consult a healthcare professional. They can assess the severity of the condition and discuss treatment options to improve sexual functioning.
- Psychological Impact: If phimosis is causing significant psychological distress, such as feelings of embarrassment, self-consciousness, or affecting self-esteem or relationships, it is advisable to seek professional help. A healthcare professional or counselor can provide support, guidance, and address the psychological aspects related to phimosis.

Frequently Asked Questions
Q1: Can I have sex if I have phimosis?
Yes, it is possible to have sex if you have phimosis. However, it may be uncomfortable or painful depending on the severity of your condition. It is advisable to consult a healthcare professional for guidance and possible treatment options to improve your sexual experience.
Q2: Can phimosis affect sexual pleasure?
Phimosis may potentially affect sexual pleasure as it can make sexual intercourse uncomfortable or painful. The tight foreskin can restrict movement and cause discomfort during sexual activities. Seeking medical advice and exploring treatment options may help alleviate these issues and enhance sexual pleasure.
Q3: Is it safe to engage in sexual activities with phimosis?
Engaging in sexual activities with phimosis can be safe, but it is important to take precautions. The tight foreskin may increase the risk of tearing or injury during intercourse, potentially leading to discomfort or infection. Using lubrication and practicing gentle, slow movements can help reduce the risk of complications.
Q4: Can phimosis lead to erectile dysfunction?
Phimosis itself does not directly cause erectile dysfunction. However, if the tight foreskin causes pain or anxiety during sexual activities, it can indirectly affect your ability to maintain an erection. Treating phimosis may help alleviate these concerns and improve sexual function.
Q5: How can I manage phimosis-related sexual difficulties?
Managing phimosis-related sexual difficulties involves exploring treatment options to address the underlying condition. Techniques such as gentle stretching exercises, topical steroid creams, or, in some cases, circumcision may be recommended by healthcare professionals. Seeking guidance from a healthcare provider is essential to determine the most suitable treatment approach for your specific situation.